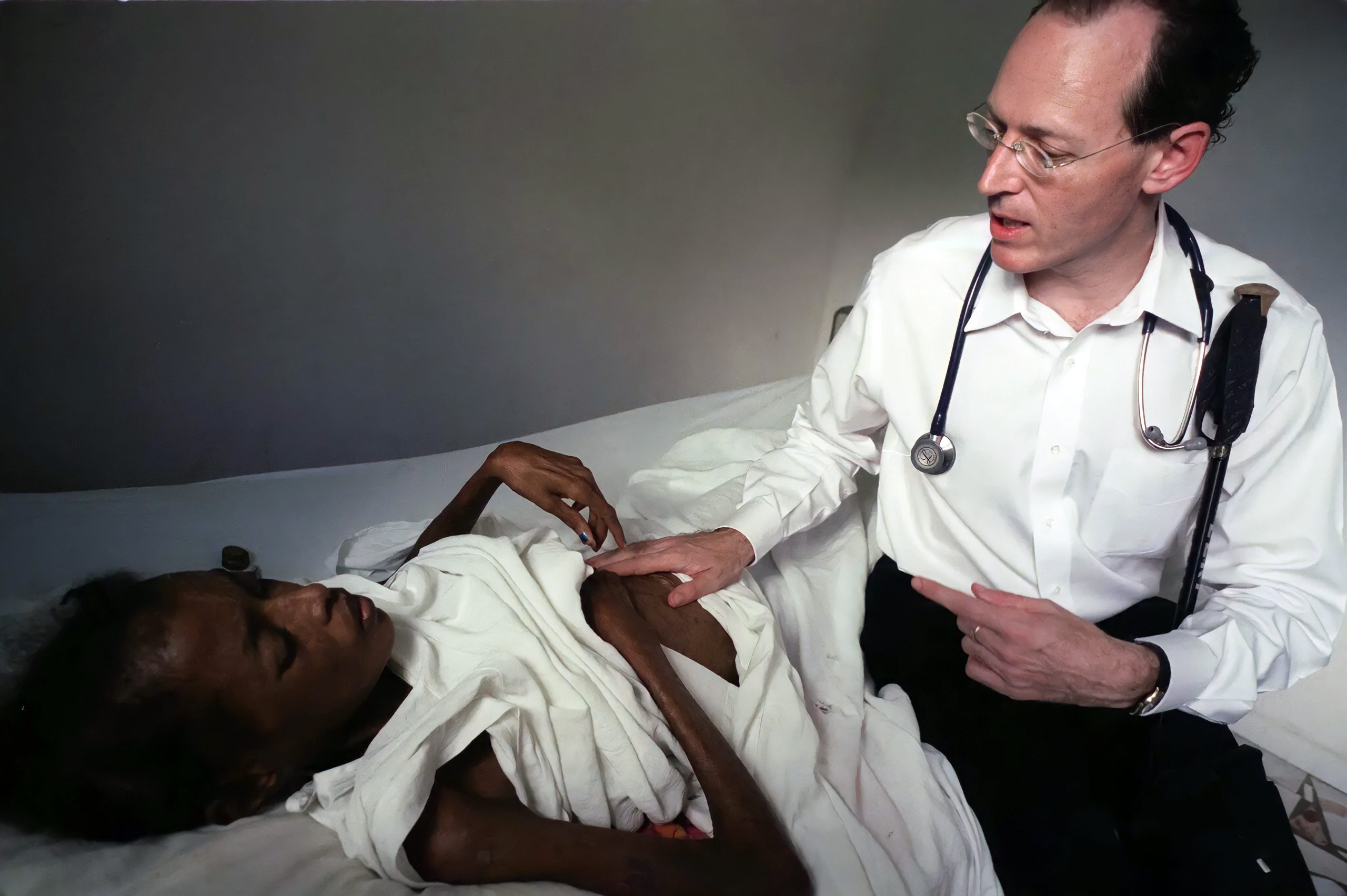
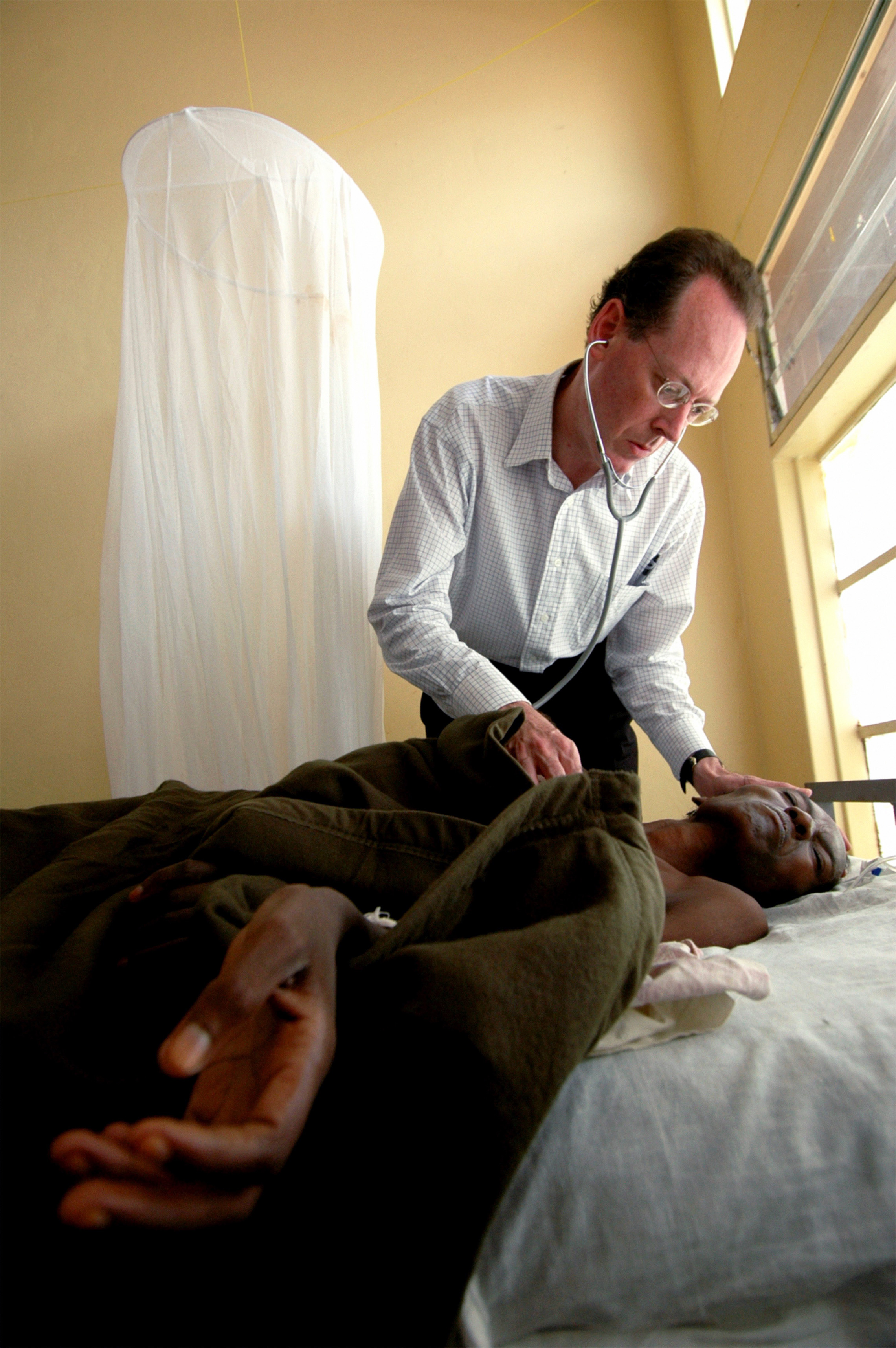
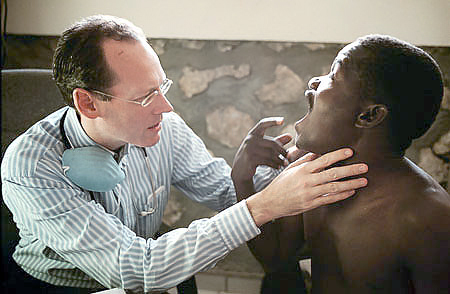
Was it on your first trip to Haiti that you learned what the building of the Péligre Dam had done to the people of Cange and the Central Plateau?
Paul Farmer: Yeah. Even now, it’s still an evolving kind of understanding. I’ll tell you what I mean. When I was 23, I went to the squatter settlement that was formed when the valley was flooded by a hydroelectric dam. So that’s one way of experiencing an infrastructure project. I was reading about the Tennessee Valley Authority, actually, of all places. Here in Cape Town, yesterday, I’m reading a book about FDR.
I studied a little bit about the TVA, as it’s called, when I was writing my first book about that part of Haiti. But the purpose of that infrastructure project in the Tennessee Valley was a poverty alleviation project, and to generate cheaper power in Alabama, Tennessee and the American Southeast. And that was the stated purpose of that dam, the Péligre Dam. It was to control the flood waters down river, and later to generate electrical power. Now remember what happened in Haiti last year — so this is 26 years later — was terrible floods. Four hurricanes hit Haiti, and some of the areas where we’ve worked, the real problem was flood control with the dams. So 26 years later, I’m thinking, “Wow, it’s still very important to have flood control if people in these flood plains are gonna be protected.” And guess what Haiti needs more of? Electrical power. So I’m only saying all this because I’m not against hydroelectric dams, but when I was 23, I got to see what poor planning of a development project meant to poor people. So it was poorly planned in terms of what would happen to the people in the flooded valley, and they’re the ones who introduced me to — the people living there — they were the ones talking to me about what this development project meant for them.
Someone asked me once, “Do you have something against dams?” I said, “What are you talking about?” and it’s just that the first look that I had, as a young American, at a big infrastructure project was through the eyes of people who had lost their land. And I think that’s a very valuable way to look at a major infrastructure project, you know, through the eyes of the people whose lives are disrupted. Now the Tennessee Valley Authority — I don’t want to sound pedantic, or like a professor, but you know, a lot of people were displaced by that project too. But it led to rural electrification and lots of good things for poor people. I think people looking back at the TVA, there’s always gonna be critics of any major project. But I think it probably was a net positive for development in the 30s and ’40s and beyond.
Whether or not we can say that about the dam you’re talking about, I’m not so sure, but we still need better flood control and more electrical power in Haiti.
Those people had no say about whether the dam would be built or not, whether they would have to move or not. What does that lack of empowerment do to the psyche of a community?
Paul Farmer: Well, I know what it does to the psyche of a community, or at least I’ve seen it. So when you’re a peasant farmer, and you lose your land, then you lose the means of supporting your family. That’s very destructive. To go from being able to work to support your family to being a squatter — a landless peasant — is a terrible and destructive thing. I don’t think anybody would disagree with that.
The question with a lot of these projects is, “Are there ways of bringing benefits like electricity, flood control, water to large numbers of people without disrupting them?” I’m sure the answer to that must be yes, and whether or not that was done there is still an open question. I think it wasn’t. Now when you talk about human ecosystems, don’t forget that Haiti is — in many ways — was created. It’s an artificial creation. The people who call themselves Haitians were kidnapped in West Africa and dragged over across the Atlantic in chains. The natives of that country disappeared before the 17th, 18th century. So the ecosystem in Haiti has always been disrupted, as is true in a lot of the Caribbean. So I’m not sure exactly how to use that term effectively there. By the time that the valley that I lived in was flooded, it was also a creation, after the Haitian revolution. People fled up to the hills. They worked the land themselves, so they were creating a new ecosystem in a sense — what you call human ecosystem— and that was disrupted again by this flooding of the valley.
Would you rather the Péligre Dam had not been built?
Paul Farmer: I think the answer to that, for me, is no. I don’t feel that way. Going back to the Tennessee Valley Authority, TVA, I may get the numbers wrong, but something along these lines. Yes, 15,000 people were displaced. I’m sure that it wasn’t done well, but think how many millions of people got electrical power — cheap electrical power — compared to what was available before from private utility companies. So I think, and I would like to look back at what I wrote when I was in my 20s, writing about — even about TVA in my Ph.D. thesis, for example. You know, I’d like to look back, and I will look back at it now that you bring it up, because I’m not so sure I was that fair to the TVA, and there are many other major infrastructure projects around the world that are, by the way, now very hotly contested, and now there is actually — there are movements against these big infrastructure projects. I wouldn’t want us to have Luddite approaches to technology and infrastructure projects. We need electricity, roads. We need green fuels. We need all those things. We need clean power. So I think we need to keep pushing forward on finding solutions to these technological problems. But we need them to be solutions that are not disruptive ecologically. We need them to be solutions that are not destructive socially. And I also think it’s fair to ask, “Well, how is this gonna affect really poor people?”
So if we could do better on that front, I wouldn’t be opposed to building a dam. I’m not even opposed to that dam. It’s just that I happened to have learned about it from the people who lost their land. It’s not about the dam. It’s about the way that those people were treated. I might add, and I have added many times in print, that they also did not get electricity or water, the people I knew. They had neither of those things. So it’s a hydroelectric dam, and you’d think the people who lost their land would at least get hydro and electric, and they didn’t. It took decades for them to get electricity.
Why didn’t they get any benefits from the building of the dam?
Paul Farmer: They were poor, that’s why. They were poor. They didn’t have much of a voice. The electricity was going off to the city, and they didn’t have the power to get the power. I think it’s good for me to read about the TVA again, 26 years later, and to look at other perspectives on what can be done — a decent, well-thought-out infrastructure that’s actually designed to help poor people. We can do that.
From Haiti, you went to Harvard and got two degrees, medicine and medical anthropology. Was that option unique to Harvard?
Paul Farmer: No, it wasn’t unique to Harvard but there weren’t many programs that had M.D.-Ph.D. programs in that field. It’s two different degrees: your medical degree and a Ph.D., and there are probably a dozen or more universities in the United States that have those programs. Maybe it’s more, but there weren’t many back in 1983-84. I started in 1984 at Harvard.
By the time you graduated, you had seen more than most medical students, because you spent so much of your time in Haiti. Haiti, you’ve said, was your best education.
Paul Farmer: Haiti’s been my best teacher. In 2005, I went to Rwanda, and along with other people at Partners In Health. There are projects in Malawi and Lisutu, with a partner institution in Burundi. So from 2005 to now, I spent most of my time — field time — in Africa. But if I hadn’t learned those lessons, and we hadn’t learned those lessons in Haiti, then how would we know really what to do in rural Africa, because those are not culturally similar places, but they’re structurally similar. So there’s no cultural or linguistic tie between Haiti and Rwanda, but they’re very poor, agrarian societies, much disrupted by political violence and with a history of heavy post-colonial burdens. So there are very significant structural similarities between those places. So of course, one hopes that the lessons learned in Haiti would be — I guess the word is “transferable,” and most of them are. So Haiti’s been my best teacher in that sense. But I wouldn’t want teachers at Duke and Harvard to think that I was saying that I didn’t have the book knowledge that I needed, that I got that in Haiti. Really, I got that in the universities. But understanding its strengths and limitations of book knowledge, if I can — or analysis in general — you learn that in a place like Haiti. You find out how far that knowledge can take you, and where you need to generate new knowledge, and that comes from working with lots of other people, as I’ve said a couple of times. It doesn’t come from oneself and books. It comes from experience, learning to listen to other people, working with big teams of people.
Tell us about the beginnings of Partners In Health. How did you come to found this organization?
Paul Farmer: The idea to start something about it came to me in Haiti, of course. I think part of it was that I saw just how many different groups had been in and out of Haiti over the years. I knew they were well-meaning, even if I was — as sometimes young people are — I’m sure I was hypercritical. That’s okay. Everybody’s a critic, and like I said, the diagnosis is easy and cheap to make, right? You know, you see all this aid money going in to Haiti. This is — I’m talking about the ’80s. Haiti’s still in trouble. It’s easy to say, “Gee, there’s a problem here.” There is a problem with the effectiveness of the aid, and there were missionary groups, and there were short-term medical missions, and there were tons of people from the United States and Europe. So I think back, then I said, “Well, we need to have long-term partnerships,” hence the name. It’s not gonna be someone coming from the United States, into Haiti saying, “Do this, do that.” It’s really about partnerships. So in many senses, certainly the idea for doing that came from Haiti, but also the start was in Haiti.
Why did you start it in Boston? To be near Harvard?
Paul Farmer: Initially it wasn’t in Harvard at all. I’m not sure that we would have anticipated that it would fit in a research university. I wouldn’t have guessed that when I was a medical student. And so I’m afraid it was quite conventional to start with. There was the notion that you needed partnership. Again, it’s not rocket science. The notion that it would need to be long-term? Not particularly rocket science either. The notion that you have to link a resource-rich setting like Boston or Harvard? That was obvious too, because all of us who were doing any kind of connection were living links between a world of great poverty and a world of affluence.
So those things were pretty obvious, I think. But building that into a series of institutions which would later span all these countries in which we’ve been working, the idea was… what we need to do is build local capacity. Again, these are almost clichés now in development work. So that meant a Haitian organization, or in Rwanda that means a Rwandan organization, or in Malawi a Malawian organization, et cetera. And that’s what we try to do, was to say, “It’s not about us. It’s not about our own quest for personal efficacy.” And again, this may be a lesson that’s worth sharing with people who would look at your website is, “It’s gonna feel like it’s about you, and your own quest for personal efficacy, or discovery of yourself, but it isn’t about you. It’s really about the people that you’re serving.” Those are hard lessons to learn, because — I don’t think — I’m not just talking about young Americans, but I’m saying, in general, young people who are achievers, who get to go to school, who could even have a computer or electricity, it really puts — hopefully, I hope that we’ll soon see laptops all over the world, and that poor people also have access to information technology. But right now we don’t have that. We have this digital divide.
So to get back to your question about the seeds of PIH, the obvious stuff, it needed to be long-term. It needed to be about partnerships. It needed to be about local capacity-building. Those are still serious problems in the arena of development.
Who is Tom White, and what role did he play in starting Partners In Health?
Paul Farmer: Tom White is a Boston businessman who gave money to a local anti-hunger charity in Boston for Haiti work, probably in 1983. That was right around the time when I was going back, to interview at Harvard Medical School. I went to this charity and said, “We need to build a bakery in Haiti.” That actually was probably not a good idea, but that’s okay. We meant well. It’s not okay to keep doing the wrong projects, but at that point, it seemed like a good thing to build a bakery. He had given this gift anonymously, and we went and built a bakery. He was the anonymous donor and that’s how I met him. He’s one of the founders of Partners In Health, and we’re still working together to this day.
From the original project in Haiti, Partners In Health expanded, first to Peru, then to Russia and Africa. How did you become involved with Russia’s drug-resistant tuberculosis project?
Paul Farmer: I went there on a mission myself in the late ’90s. There weren’t that many people in the world who were still focused on that clinical problem of drug-resistant tuberculosis. There’s a few centers in the United States, one of them in Denver, but there are not that many. Tuberculosis is not a huge burden in the United States. There’s a debate over how much TB there had been in Russia in the ’80s.
It’s clear that TB started making a comeback in Russia, after the collapse of the Soviet Union. It was a prison-seeded epidemic, just as we’d had in the United States, in New York for example, in the ’80s. A lot of these epidemics of drug-resistant TB started in prisons or homeless shelters in the United States. The same thing happened in Russia, and I had that particular clinical training and interest, so that’s how I got involved. How we got involved as a collective was — we thought, “Wow. There’s — again — people of goodwill here: the prison health officials, the doctors and nurses. There’s a great need. Some of the tools that are needed to respond effectively are not available. Could we get them there? So all that came together to lead us to, to start another Partners In Health project there.
Russia wasn’t the first place Partners In Health went after Haiti, but was Russia part of an expansion —a globalization — of your outlook on infectious diseases like drug-resistant tuberculosis?
Paul Farmer: We’d always had a globalized view of these epidemics. The question is, how much could we be effective globally? A lot of groups, I think, overshoot. They try to do too much, small groups. They try to say, “We’ll do this for the whole country or district.” We didn’t want to do that ever. We still don’t, as Partners In Health.
We knew that these were transnational epidemics, transregional, globalized epidemics. The same is true for lots of other pathogens. We knew that, but the question was, “How could we be effective?” And the way that we got started was working with the Open Society Institute, which George Soros founded. And then the Gates Foundation, in one of their first major delivery grants, started supporting our work in Peru. And we went back and said, “Look, you know, there’s a very big problem in Russia as well. Do you think we could help there?” So we ended up re-formulating our support for the Peru project, to support Peru and Russia, to really scale it up in Russia. So yes, in a way that was an acknowledgement of what we always knew to be a globalized problem. How could it be otherwise? it’s an airborne disease, so it’s going to spread, globally, just like swine flu or SARS.
You’ve done so much work with this problem of multi-drug-resistant infections, such as tuberculosis, what we call MDR-TB. Could you talk about that specifically?
Paul Farmer: I’d be glad to, and I think that’s important. I mean, look where we are. We’re in South Africa. It’s a huge problem in this part of the continent and it’s not been acknowledged.
How did this come about? Is this a case where the solution to the problem became the bigger problem?
Paul Farmer: Did the solution become the problem? I think the answer is no. Everybody thinks that, but putting it that way allows me to lay it out. It’s not just about TB. It’s about staphylococcus, HIV and every kind of infection. In general terms, there’s the bugs and there’s us. And the bugs, these are human pathogens, they’re the enemy, all right? And I’m sorry I can’t be completely touchy-feely about that. These are bugs that kill humans. They’re viruses, parasites, bacteria. I don’t have anything against dams, and I don’t have anything against microorganisms, unless they’re pathogens to humans. That’s the link here. If dams help people, I like dams. If bugs don’t hurt people, I’ve got nothing against bugs. They’re all over us and all around us. But these are pathogens that kill millions of people every year.
The general point is, humans in the mid-20th century began to develop an arsenal of anti-infectives that could kill bacteria, parasites and viruses. It took a long time, and it’s still ongoing, but that’s the basic development. In the mid-20th century, we started getting the weapons we needed to kill the bugs that were killing us. But what happens is the bugs fight back, and they develop resistance to the weapons. So — and then let me give it — before even talking about tuberculosis, ’cause it’s very contentious. Why? ‘Cause it’s airborne, that’s the main reason it’s contentious. But take staph aureus. Everybody hears about killer staph. It’s a terrible pathogen. In the mid-20th century, almost all of the staph could be killed by penicillin. Now, 95 percent in South Africa and in the United States, it’s all resistant to penicillin. So the bugs can’t really be killed by the drugs that we developed in the 20th century. So we’re playing catch-up. Now that’s the general issue. I mean, you look at malaria, you look at TB, you look at HIV, you look at bacteria, like staph. It’s a general story.
The bugs are going to fight back. They’re going to develop genetic mutations that will allow them to escape the killing by the antibiotics, the anti-infectives. So it’s not just about one disease or another. So the question, the way you put it, which I think is the way most people ask, “Is the solution part of the problem?” And I would say, “No, that’s not the problem. The problem is the way we use the solution.” So go back to TB again. If we had had a way, in the mid-20th century, of delivering effective therapy for tuberculosis to everybody who needed it, then we would have had community health workers, and all these things that we have scrambled to development, I don’t think we’d have the big problem we have today with drug-resistant tuberculosis, MDR-TB.
Why didn’t we do that? Why do we have this big problem?
Paul Farmer: ‘Cause we keep trying to do it on the cheap. What do I hear all the time in my work? “We can’t pay community health workers ’cause it’s not sustainable. It’s too expensive.” When what’s really expensive is to not pay the community health workers. That’s what’s really going to get you in the end, to have cheap solutions for really complex problems. For example, in the United States, with HIV, with AIDS, if we would simply put in place good community-based care and actually pay community health workers, then we wouldn’t have so much drug-resistant HIV. Same in South Africa. What we’ve tried to do in our work with the so-called public sector, with the Ministry of Health in Rwanda and Haiti, is to say, “Now let’s do it the right way from the beginning. Let’s start by making sure that people who are sick have access to care, and that it’s supervised by community health workers who are living with them, in the same villages.”
This conventional model is, the patient’s sick, they go in to the doctor. But there are no doctors out in rural Haiti. There are now, but I’m saying that was not a viable model, and so we actually developed a different model, that turned out to be better then the standard model, because it actually delivered good community-based care. We say, “free of charge to the patient.” Okay, maybe that’s not the right term, “free of charge.” ‘Cause obviously someone’s paying for it right? Someone’s paying the labor costs for the community health worker, the diagnostics for the lab and the medicines. But if you don’t want to see this drug resistance develop with the chronic infectious disease, then don’t ask the patient to pay for it. Because when they have money, they’ll pay for it, and when they don’t, they can’t. And then the treatment gets interrupted, et cetera, et cetera. The whole chain inevitably leads towards drug resistance.
To be very clear, what is happening on the ground level that is creating this drug resistance? What is it about healthcare and the infrastructure?
Paul Farmer: You’re right to push me on this. I’ve studied this my whole life, and this is my reading of it. I think this is what’s happened. Of course we wouldn’t have drug-resistant disease if we didn’t have antibiotics. We would, but they’d be naturally occurring mutations that didn’t add up to much in human populations. So it is true that the challenge of antibiotics is what created drug resistance to start with, and spread it through human populations, that’s true. But I would say there are other causative factors here. For example, the model of care that I described. You have someone who pays. If they have money, they pay for the treatment. Is that the right model for public health? I don’t think it is for infectious disease. In fact, I don’t think it’s right for a lot of things.
Healthcare in the United States is very expensive, and part of the problem is it’s very expensive to give bad medical care to poor people in a rich country. Think about that. It’s expensive to give bad medical care to poor people in a rich country. We’re in Cape Town, so let’s just talk about Cape Town. You look at the massive teaching hospital here, or the beautiful university, but you know, the idea that some people, because they’re poor here, are not going to try and get good medical care for their family, that’s absurd. Of course they are. Women who live in poverty love their children just as much as anybody else does. So you’re going to have all of this engine of really effective connections, and families are going to push people to try and get medical care. But if it’s a commodity that you buy, then when you’re poor, you buy it sometimes, you can’t buy it at other times. That’s not a good model for public health response, I would say.
So a lot of people figured this out around tuberculosis back in the 20th century. They said, “Oh, we made a mistake here, selling these drugs.” So they took the drugs out of the pharmacies and put them in the hands of public health officials. I think that was the right thing to do. The problem is, in the world, we don’t have that system set up in enough places so that everybody who has tuberculosis has access to diagnosis and care. Instead, they don’t know what they have. They cough. They go get a chest X-ray. They pay out of pocket for that. They’re told one thing. Maybe they get good advice, maybe not. But that system, globally, is not set up very well yet.
Isn’t that the definition of bad medical care?
Paul Farmer: Yeah, but the doctors and nurses who are delivering bad medical care aren’t doing it on purpose. If they don’t have a system behind them, what can they do? In The New York Times Magazine last week, the last page, there’s a one-page essay. It’s about an American woman in India. She has had a problem with a malignancy, a cancer, in the past. And she’s told by her American doctors, “You can go to India, as long as you have some screening now and again.” So she hooks up with this doctor, and he is this cheerful fellow who really has nothing to work with. And at the end of that one-page essay, they go and visit this Indian woman who’s dying of cancer. And he’s saying to her, “Be of good cheer,” and the American said, “It seemed cruel, but that’s all he had, was words.” And that’s it.
The doctors and nurses who are delivering mediocre medical care are not doing it ’cause they want to. They’re doing it because they don’t have the tools of the trade, the system behind them that they would need to provide good medical care. You know, in all the years that I’ve spent working in Haiti and Africa — which is now 25 years, and Latin America — versus, say Harvard, I tell you, I don’t think that these young professionals in Africa are any less committed, even though I would have said that 15 or 20 years ago. They’re not less committed to medicine and to people’s health. They just don’t have the systems and tools that they need. One of the biggest epiphanies for me in working in these different places is, if you can set it up so that young African professionals, nurses and doctors and social workers and people in Haiti, et cetera — if they can actually do their work, they’re happy to do it. People talk about the brain drain. One of the best ways to respond to brain drain is actually give these young professionals the tools that they need to serve the poor, ’cause they’re surrounded by the poor. I think that’s a big part of what we need to do in global health, is to make sure that we don’t make the mistake, say as young Americans — I’m not young any more, but — of saying, “Oh, it’s all about us going in and saving the day.” It was never about that. It’s always about building systems, and building teams, and building partnerships that will last.
So drug resistance is, in a way, a big challenge to the “healthcare as commodity” approach to healthcare, which is this sort of garden-variety approach. If healthcare is something you buy, what if you’re poor and you have an airborne disease? What if you have influenza or tuberculosis or swine flu? Who knows? If we don’t take that as a public health problem, it’s just a private problem, and then it’s going to be out-of-pocket expenses, and it’s not going to be the right response to these kind of problems. Same thing for malaria, and on and on it goes.
Do you see every pediatric death in Haiti as a failure?
Paul Farmer: Well, sure. It’s somebody’s failure, right? What’s the normal lifespan of the human right now? Say 80 years old. When I say normal, I meant if you have those things that one needs, like clean water, and vaccination against preventable illnesses, and education, and you’re not caught up in some dreadful conflict. Why shouldn’t you see grandchildren, right? That would be the normal course of human events if you have those things. So do I see every Haitian pediatric death as a failure? It’s somebody’s failure, usually, right? Same in Burundi or India or Cincinnati or wherever. I don’t think it’s a bad thing to see failure as failure, but it’s important to understand how to assess causality. I know in some ways it’s better to keep it simple, but claims of causality are really difficult to make. They are seldom buttressed by really sound data. If you say, “a” causes “b,” then you ought to know how causality is created. For example, there are papers that ask, “Why do poor people behave poorly?” It’s really a talk about causality. What drives behavior? Here we are in Southern Africa. We’re talking about epidemic diseases here, but they’re really caused a lot by labor migration. People don’t talk very much about labor migration. Public health people don’t talk about it very much, because they’re not trained to talk about it. Medical people even less so, because they’ve had even less training. What I’m saying, and this sounds kind of wonkish, is large-scale social forces determine a lot of these things, including pediatric deaths.
So when I say, “Yeah, sure,” it sounds dramatic to say, “Every pediatric death in Haiti is a failure.” But it’s true. Somewhere along the line, there’s a failure. How else will we explain it? If you go to a place where infant mortality is, let’s say, 150 per 1000 — 150 children die in their first year of life — there’s got to be failures. So what are they? Well, they’re a failure to vaccinate. They’re a failure to make sure people have clean water, et cetera. So I think it’s really a good thing to — not so much assign blame — but to assess why things are failing. It’s also a good thing to take responsibility for that. So I don’t see it as my personal failing when some kid dies in Oakland or Okinawa, but it is a failure. And I think it’s probably better to think of it as our failure, not because we’re into sack cloth and ashes, but because we’re trying to fix fixable problems. So it’s really, ultimately, a very optimistic thing to say, “It is a failure.” I’ve thought a lot about this over the years, optimism and pessimism. When you say, “Hey, that’s a failure,” it’s ultimately an optimistic kind of engagement, because you’re saying, “That could be fixed.” But if you say, “That’s the way the world is,” or “That’s life,” or “That’s destiny,” well, that’s not so instructive in terms of having an action plan.
Students who want to go into public service or healthcare, or who want to serve in rural Haiti or Rwanda, might think they need degrees in medicine, cell biology, infectious diseases, foreign affairs or international policy. But how can business majors be useful in a service sector?
Paul Farmer: I think that’s a great question. There’s another widespread misperception here, is that in order to be involved in these kind of problems, you have to take certain kinds of training. That’s just not true, because as we said at the outset, we have all of this array of social problems. But let me just go back to business majors, for example. First of all, the problem is very often delivery, right? Let me put it in the most general terms. Do we have a vaccine for polio? Yes. Is it effective? Completely, or pretty much completely. So why do we still have polio in the world? ‘Cause we haven’t gotten the delivery down, and sometimes in speaking about these problems, you can talk about, “Discovery, Development and Deliveries.” So discovery is something that happens in the lab, right? Often, and the polio vaccine comes from basic science research. And development — you develop a product — that can be done lots of different ways. Pharmaceutical companies develop products, for example. It’s the third “D.” It’s delivery — the implementation — that is the biggest problem. And not to single out any company — I don’t really know much about companies — but FedEx has to deliver their — they have to get the thing there. And I think we need to take a similar approach to global health and development as, “We’ve got to deliver.” We have to have ways of assessing how effective we are at delivering.
You mentioned business school and you mentioned business. There are clearly skill sets from the business sector that are important in public health and public good in general, like education, clean water. A very “big tent” approach is what we need for these problems. They’re complex social problems, they have complex social answers, but we’re going to have to have a very big tent. We’re going to need those cell biologists and other basic science researchers to develop the tools. We talked a little bit about tuberculosis, but one of the biggest problems with tuberculosis is we don’t have diagnostics. We don’t have the tools we need to diagnose the disease. We don’t have a vaccine, so these are basic science questions as well. So we have to do that, and then we have to develop these tools so they’re available. Finally, and this is what I work on in a lot of Partners In Health projects, we work on the delivery side, taking these innovations in science and public health and delivering them.
They say doctors make the worst patients. Yourself included? What have you learned from getting sick yourself?
Paul Farmer: Drink clean water. I tell all my students that. Drink clean water.
Have you ever gotten so tired of system failures and losing patients that you lost hope?
Paul Farmer: No, I have not. But that’s because I work with thousands of people. If you ever make the mistake of thinking that you’re going to do something on your own, then you will learn the hard way that that’s never the case. Maybe if you’re a painter or a poet or an artist or a writer, but work in public health — and public education and public good — requires teams. Teams have to shore each other up. That’s an important part of this work. You’ve got to work as a member of a team.
Do you remember any setbacks along the way that turned out to be invaluable learning experiences?
Paul Farmer: Yeah. For example, to lose a couple million people every year to tuberculosis. But then there’s this question, as I said earlier, “How do you assess failure?” How do you understand why a treatable disease becomes so lethal? And understanding that, in my view, requires lots of talking to patients, their families, the health providers, et cetera. And some of the things that we saw in the ’80s, really, they were failures, because patients died. But they allowed us to diagnose the systems’ problems and say, “This is where we need a community health worker system. This is where we need to make sure patients have food support while they’re getting these medicines,” et cetera. So those are examples of tragedies that certainly lead to — not just personal epiphanies — but collective epiphanies, where you say, “You know what? We can do this better if we have the system fixed.”
You’ve spent so much time with the poor and the suffering in Haiti. Do you find a different paradigm in Haiti than you do in Peru or in Russia?
Paul Farmer: They’re all different paradigms. New Jersey versus Peru versus Haiti. So everywhere humans hang out and develop cosmology, ways of explaining the world, there’s always different ways of explaining misfortune, right? So yes, always different. But one of my questions is, “How much time do we spend looking at that, when we could address system failures and rebuild better systems?”
Do the system failures present similar paradigms?
Paul Farmer: Yes. The system failures require similar paradigms. The explanatory models vary enormously. So in Russia and in Rwanda — which have no similarities — or in Boston, the system failures are that we don’t have a good enough community-based support for adherence. Those are system failures. But people’s explanations of their suffering varies. It’s all over the map.
Why were Haitian women working as servants in Port-au-Prince more at risk for contracting AIDS than women who stay on the Central Plateau?
Paul Farmer: I mentioned labor migration already, and this has happened all over the world with urbanization. Stable social networks, like families, get disrupted, right? I keep referring to South Africa, because we’re in it, but that’s what Cry the Beloved Country is about. That’s happening all over the world. You look at the 19th century, and there were lots of rural communities that had their own kind of stability, and those were disrupted by urbanization and industrialization, and there’s a lot of social pathologies with that. Now humans have to ask, “Is it worth it, the technological progress and advances?” I guess the answer is yes. That’s why people are voting with their feet and moving into cities all over the world. But there are consequences, and that’s why we have written a lot about gender inequality and poverty, and how they work together to increase risk for certain pathogens like HIV. I know that’s a kind of longish answer, but it takes a long time to describe that.
In Rwanda, you encountered the phrase “Charity Industrial Complex.” What does that mean?
Paul Farmer: I got that expression from a series of articles in the Rwandan newspapers. One of the Rwandan newspapers had a three-part series about the Charity Industrial Complex. It’s a blistering critique of NGOs and foreign aid, looking at how it’s structured and how there’s a lot of overhead. And there’s not enough local capacity-building, and there’s not enough coordination. So it’s a critique really of NGO performance in Rwanda, and I think they have the right to be critical of what’s going on in their country. I think it’s very important for those of us involved in working with NGOs to understand the critique that is being made of our effort. That’s what the authors of that series of articles called it, “The Massive Rise of NGOs in Rwanda and Across Africa is the Charity Industrial Complex.” Sobering.
What do you think is the chief barrier to developing healthcare in rural Rwanda?
Paul Farmer: The chief barrier? It’s not lack of people to work. It’s not lack of need. There’s lots of unemployed people, or underemployed people. So you can’t say, “There’s no one here to work.” That’s not true. It’s not lack of need, because there’s clearly a lot of need. I would say that it is, if we can move some of these resources out of the cities, and into the rural areas, and into job creation, for example, for community health workers and community teachers and community agriculture agents. If we could move some of those resources out there, we’d really get a big leap forward in breaking this cycle of poverty and disease. That’s what we’re talking about, is a cycle of poverty and disease. People are trapped in it, right? Some people call that the poverty trap, but how do you spring that trap? How do you break that cycle? I think job creation’s a big part of it. One of the things I see as the chief barrier is that we’re not committed enough yet to job creation in these areas. Now initially what we’ve done is to create jobs in healthcare and education, but you also need generative jobs in manufacturing. It can’t only be healthcare and education. There have to be other jobs as well.
Before I can create a job, if I’m an NGO, I’m contending with funding and cultural skepticism…
Paul Farmer: I think it’s more funding. I don’t think that “cultural skepticism” will work. Why would there be people in Rwanda writing articles called “the Charity Industrial Complex?” Because they’ve seen lots of development assistance, but it hasn’t been effective enough. If we can make that effective, then that would go a long way to easing that skepticism. I’m not saying anything original. First of all, I’m echoing and amplifying the views that I hear in Haiti and Rwanda. I’ve heard these critiques many times. But there’s also a book. A guy named Peter Uvin wrote a book called “Aiding Genocide” (Aiding Violence), I think is what it’s called, “Aiding Genocide.” And it’s really about the way in which the development machinery helped set the stage in part for what would happen in Rwanda in 1994. It’s not blame. The claims of causality, again, are important. He’s not blaming the Charity Industrial Complex, but he’s saying, this is part of the problem. So that has led to a lot of skepticism. But I’m an optimist. I think we can turn that around. We can make aid more effective, and have better metrics for assessing the effectiveness of aid. And I think that’s an area that would be supported by everyone. It’s not a partisan kind of problem. Everybody should want aid to be more effective.
It’s really not only, it’s a quest for funding — there’s a lot of money going into aid — the question is, “Is it being used as wisely as it can?” Do we have the right ways of assessing its effectiveness? I don’t think we have the right ways yet, and we can certainly develop them.
If Rwanda becomes self-sustaining in healthcare, what will we be looking at next? Where will we be developing healthcare ten years from now?
Paul Farmer: I think the public sector has a very big role to play. But we want the innovators and entrepreneurs, that’s part of the reason I’m speaking to you here today. We need the young generation to be engaged, and they are engaged. They’re engaged in public health and public good, much more than I saw in the ’80s when I was a student. So we need that. They’re the people, just in terms of the temporality, time-wise. We’re not going to be doing it, it’s going to be the people who are young now and studying this now. But they also have to find a way to engage the public sector, that is, the public health sector, the public education sector. That’s not easy to do, because it’s easier in a way just to be an NGO and go it on your own. But that’s not going to be a long-term solution.
You became involved in these issues at such a young age. Going back to your childhood, where were you born and where did you grow up?
Paul Farmer: I was born in North Adams, Massachusetts, in the Berkshire Mountains, and I grew up mostly in Florida.
Didn’t you spend a little bit of time in Alabama?
Paul Farmer: I did. I don’t want to leave out Alabama. I lived in Alabama for a few years. I started elementary school there, in Birmingham.
What was school like?
Paul Farmer: I went to the public school in the neighborhood for the first few years, and then I went to a magnet school in fifth grade. It was really a great program. So I have all these very good memories of Alabama as well.
Could you tell us about your parents?
Paul Farmer: My parents met in North Adams, Massachusetts. My mother is from Williamstown, which is right around the corner, and my father was from North Adams. They met in college, in what used to be called Teachers College, where people train to become teachers. That’s where they met.
What brought them to Birmingham, Alabama?
Paul Farmer: My father was looking for a job, and he had heard of something in Alabama. We were kids at the time, so we were not involved in the decision-making. And that didn’t work, so he went back to teaching.
When you say “we” were kids…
Paul Farmer: I’m one of six kids, so it was the eight of us. I’m number two of six. I have an older sister.
When and why did the family then go to Florida?
Paul Farmer: It was a difficult time in that city. My father was a public school teacher, and he thought the environment was tense in Alabama, in the late ’60s, early ’70s. He just decided we would try again in Florida, so off we went.
As a kid in Birmingham, did you understand what your parents were trying to escape?
Paul Farmer: I didn’t really sense too much of the trouble. I was eight or nine or ten years old. You’re sheltered, even though you’re in schools, so I wasn’t alive to a lot of the tensions at that time, which were largely racial tensions around the civil rights movement. My father was a high school math teacher, and it was a difficult time for the United States. I think he wanted to shield his kids from that kind of tumult, so off we went to Florida, and I stayed there until I went away to college.
What kinds of things did you do in Birmingham, besides going to school?
Paul Farmer: Personally, as a kid? I was very interested in science and in reading. I was kind of a nerd. I was just doing what kids do in elementary school. I was going to school, hanging around with my brothers and sisters, spending time reading. I spent a lot of time reading.
Did you join clubs or Scouts or teams, or did you gravitate toward solo activities?
Paul Farmer: No, I didn’t really gravitate towards solo activities so much. I did the whole sports teams. That was really not my bag, though. I really liked school work and reading a lot. I got really involved in reading in fourth — fifth grade. That was really my escape, and what I liked doing most. But I was very gregarious. You live in a big family, with eight people around all the time, and you just, you become part of the social unit. Since my father was a school teacher, we had three months off. So he ended up buying a bus, which initially, we were going to go off in it. He made it into a camper. The first one he bought was a school bus. It looked like it was a yellow school bus. And he just literally spray-painted it and ripped out the seats and put in bunks. And so we would head off. We’d go to Massachusetts to see our grandparents. My father also went back to college to study more math at the University of Vermont. So we’d head up north, and then we got a bigger and better bus which was — this is one of the ironies — it was actually a bus used for screening tuberculosis. So it had an X-ray machine in the middle of it. I mean it seems bizarre that I would later become a tuberculosis doctor, but who knew then? I was only nine or ten. And the area where the X-ray machine — they took out the X-ray machine, and that’s where my father built bunks for the three boys. And then one year he just said, “You know what? We’re not going to back to Birmingham. We’re moving.” And so we lived in the bus for years, eight people. So you asked about solo activities. Not too many when you’re eight people in 28 feet of space.
You say you were in fourth and fifth grade when you really got hooked on reading. Was there something you read at that age that particularly excited you?
Paul Farmer: I had these friends. I remember their names, the Crutchers. They owned a bookstore in a place that’s now — I went back to look for it — it was called Five Points. It’s still there, but now it’s the medical area. They had a bookstore, and I went to school with two of their sons, who were twins. They used to give us books. We used to be able to go hang around the bookstore. And I remember one year, I think it was my tenth birthday, they gave me Lord of the Rings, three books in a row. And you know, I just really started reading a lot from the time I was ten on. So yeah, that was a whole new world once you really start. And it’s wonderful to see kids — like my daughter is so into reading now, my older daughter. It’s just wonderful to see how that opens up universes for children. It’s really great that there’s so much reading going on now. But that was it for me, that was my fifth grade, ten years old. Never looked back. Always been a reader since then.
Did your parents encourage you? Were you a gifted child?
Paul Farmer: I’m not sure I understand that term anymore, because I meet kids in Rwanda or Haiti, or all over the world, who clearly are gifted, but they might not have the chance to go to school. So that kind of notion has been a little bit bankrupt for me, now that I see what it’s like in the rest of the world, where the kids don’t get a chance to go to school. I had the chance to go to school, and to get books and to read. That was great for me, and I’d like to see other children have that opportunity as well. My parents definitely encouraged all of us to enjoy school and to read. After all, my father was a school teacher, and my mother would have been a school teacher if she didn’t have all these kids. That’s where they met. So yeah, they encouraged us.
Was there a teacher or a mentor who opened up new opportunities or challenged you?
Paul Farmer: I had teachers like that every year.
I mentioned fifth grade, ’cause I had a school that, for that one year, really focused on challenging kids. We made a television show. We started learning other languages. It was great. But I actually got that all the way through, first grade on. I think that’s another thing I’ve come to appreciate more, as a teacher myself, is how hard public school teachers work to engage 30 kids. It’s not easy to do. They all feel, their parents are sending them off, you got to go to school. And some of them are going to be more interested than others. So I have a deepening respect for what public school teachers do. Junior high, high school, elementary, all of it. So I got that all the way through.
I had lots of teachers encourage me. And I still know some of them, my high school teachers. But one of them encouraged me. She said, “Well, what do you want to do?” I said, “I want to be a doctor.” And she asked me where I wanted to go to school, and so I named all the Florida public universities which seemed within reach, financially. And she said, “Well, maybe you ought to apply to Duke, and maybe you’ll get a scholarship.” And I did both those things. I applied and got a scholarship. Her name is Wendy Tellone, and she’s still involved in public school teaching. I think she’s still in Florida. I saw her and was able to thank her and some of my other high school teachers last year. I have been looking back. I realized, again, that people teaching public school go in every day and have a bunch of unruly and probably surly kids to engage. It’s not easy work. I’m full of respect for them now. I may not have seemed that way when I was a kid.
So what year did you go from Birmingham, Alabama to Florida? You went by bus?
Paul Farmer: Yes, by bus, and stayed in the bus. I had finished fifth grade, so sixth grade. From sixth grade I stayed in the same place in Florida.
Why Florida?
Paul Farmer: My dad was looking for a job, somewhere quiet, and we had been there on vacations — spring — in the bus. We all thought it was a pretty cool place, the Everglades for example. So he got a job in the public school system in Hernando County, and off we went. And we went into, as one does with a bus, we went to a campground, which was supposed to be temporary, and then it wasn’t temporary. I mean, when I left for college, it was still in the bus.
Did your family buy a boat?
Paul Farmer: Yes. My dad got these — they were called sealed bids. How does the government get rid of its surplus? Like a car, a military vehicle or a boat. He would look at these all the time. I remember one year he bid on a car. The stipulation was he had to spray paint over the side that said, “Property of U.S. Army” or something like that. I remember exactly how much he paid: $280. That was the car. And that’s how he got the boat. So we had a boat that was from Jacksonville, shipped down to the Gulf Coast, and soon we moved from the bus to the boat. So let’s just say, from the time I was ten, until many, many years later, I never lived in a house. But living on a boat was cool.
Why was living in a boat cool?
Paul Farmer: Because that part of Florida, the coast of Florida, it’s very wild. It’s like the Everglades. Beautiful.
For a kid who’s into science, what did that do for you?
Paul Farmer: At that point, my interests in the natural world were well set, but I enjoyed it very much, being in that part of Florida. It’s a stirring countryside, where a bunch of fresh water estuaries meet the Gulf Coast, and it’s full of all kinds of wildlife. It’s just beautiful. Not the kind of place you want to stay for a long time when you’re 18, but it really was very beautiful, a good place to go back to.
How long did your family stay on the boat?
Paul Farmer: Some years. I left in 1978 to go to Duke. But they were there for a while. They were between the bus and the boat, but then we moved the bus to where the boat was.
Did something happen to the boat?
Paul Farmer: Yeah. We had to move, and the boat went on its last voyage. I was not around then. I had just graduated from college.
What was high school like in Florida? Were you challenged academically? What kind of environment did your high school provide?
Paul Farmer: I’ve already said I have a respect for public school teachers. I think it’s difficult, you’re trying to appeal to whoever shows up in the public school system. I think at the time it might not have always felt challenging, but for people who are working hard, and who can focus on the academic stuff, it’s plenty challenging. But how many teenagers actually do that, stay focused on the academic stuff? I didn’t very much, but I enjoyed living there, and being part of the high school scene, and I learned a lot. Then I looked back, and learned about things that I didn’t learn then. Maybe I got started on that path in high school, in Florida. So I don’t have any complaints about it.
Did you do well academically?
Paul Farmer: There are other people who worked a lot harder, but I was lucky enough, like I said, to get to Duke, and then things opened up, ultimately, really very dramatically for me to go to a research university. That’s when I really started drawing on my interest in reading, and not just science, but everything. So really the whole world opened up for me at Duke. I’m very grateful. Most of the things that I’m doing now, the kind of medicine I’m interested in — I ended up doing graduate school in anthropology — all that started for me at Duke, even getting interested in Haiti. I started writing for the school newspaper. So when I go talk to university students, like some of the people who’ll be here, when I say, “Look, this is a great time, this is…” — it sounds so like a cliché that a professor might say — “…this is the best years of your life. You’re in this oasis of privilege.” But for me, that was very much the case. So I can say to them, “This is a time when you really can build interest in everything from fair trade to whatever academic interests you might have.” That’s what happened to me at Duke.
Was your family religious?
Paul Farmer: Not really, no. My grandparents, my grandmother was, but not so much my dad. He was a free spirit.
What kind of jobs did you have as a teenager, and what did you spend your earnings on?
Paul Farmer: I worked a lot. I remember I worked at a grocery store, as a bag boy, all that stuff. But I spent my earnings on books, often.
Didn’t your father and your brothers and you pick oranges?
Paul Farmer: Oh yeah, way back. Yeah, we did. My father had the boat, and he said that he was going to become a commercial fisherman, which sounded cool, and he never succeeded at that, but this boat looks like a giant rowboat, it just was empty. So we had to build an infrastructure on it. We needed cash. That didn’t last too long, though. Let me tell you, that’s hard work.
Who did you meet? Who else was picking oranges?
Paul Farmer: We didn’t really meet people, but there were people coming from Mexico, from Haiti, from all over the Caribbean. But we didn’t last long doing that.
Was that the first time you met people from Mexico and Haiti?
Paul Farmer: Probably, except for maybe kids at the school. That part of Florida, it’s not like Miami or Orlando. It’s not a crossroads. It’s in the middle of nowhere. But yeah, that’s probably the first. I didn’t know how sheltered we were until much later, when I actually went to Haiti. Of course, since then, I’ve been all over the world, but I’d never been out of the country, except Canada, when I went away to college. I’d only been on a plane once, and now I feel like I live on planes.
Was there an experience or an event that inspired you most as a young person?
Paul Farmer: Not that I would point to, no. Living in a big family, you learn a lot about how to get along with other people, especially when you’re in extremely crowded circumstances. I can’t point to any single thing. I was just really lucky, it sounds bad to say, but I got to get out. When you’re living in a small town, or a village, to go to a research university and discover the world is really a terrific process.
Did you know from a very young age what you wanted to do, or was it an idea that evolved over time?
Paul Farmer: I said that I wanted to be a doctor, but you look back and say, “Why did I say that?” I had no experience with doctors. I didn’t really know any. These days, if I’m looking at an application to medical school, looking at his or her statement, I just look back and kind of humbly think, “What was my reasoning for wanting to do that?” So I’m not a real harsh critic of whatever a 22-year-old might say in a medical school application, cause I’m not sure I would have done a good job justifying why I wanted to do it. You can sort of grow into what you want to do. You can grow into your aspirations, I think. Here’s one of the examples that I give all the time.
I grew up in a very large family, in a very small space, and I’m very close to my brothers and sisters. But one of my brothers is a pro wrestler on television, and so we had the same childhood experiences. He’s now a — fortunately, no longer wrestling on TV — but I’m just saying, the idea that you have some experience that makes you into who you are — I mean that’s a very common explanatory device, but you can all come from one family and do very different things, based on the same experiences. So for me, when I said I wanted to be a doctor at a very young age, it turned out I did want to be a doctor, but the reasons for doing it may have changed over time.
Have we heard of your brother?
Paul Farmer: Probably, if you’re a big wrestling fan. He was New World Order Sting, he was Super Jay, that was more in Japan and Asia. He got around. He’s a big, big fellow.
What was your transition like — from living with your family in Florida, in a big, communal family — to Duke University?
Paul Farmer: Well, to go from a bus to a dorm, you’re still in a communal living situation. It was great. Like a lot of kids that are 18 getting to go away to college, I think it’s a terrific experience.
Culture shock?
Paul Farmer: We’re pretty resilient. A little, but not that much. You get caught up in classes, so not really. It was a radically different culture, I’ll grant you that, but remember I’m now about to hit 50, so I’m looking back and thinking, “Culture shock? What about Florida to Haiti, or Haiti to Rwanda?” So in terms of what I’ve seen in the last 25 years, no, that was not a very striking shift of culture. It’s still American culture. It was later that I learned more about what culture shock was like, not so much as a student.
Do you think your upbringing contributed to your professional mission, or do you think you were predisposed to public service? Were you hard-wired for service?
Paul Farmer: That’s a great question, but I don’t think there’s an obvious answer to it, because, like I said, I come from a large family. We all shared the same experiences, but we all do very different things. I’m not sure it’s hard-wired. I would have argued 20 years ago that it is not hard-wired.
Anybody can learn to be interested in public service, or service to others. You can learn it early or late, and I’m very much someone who encourages that kind of plasticity of engagement. You could be 80 years old, you could be 20. You can still get engaged in service to other people. So I’m not sure that it’s hard-wired, but I think you’re conditioned. Like, all of my brothers and sisters have very similar sets of expectations of the world, of what we should do for other people, I think, even though we do very different things. So is that hard-wired? Is it the way our parents raised us? Nobody knows for sure. People make very confident claims about the ideology of a certain set of expectations, that is, you’re conditioned by your environment. Yeah, but I’m not sure you know now. And I’ve thought a lot about this, looking at other people’s lives. Why do they do what they do as adults? One looks in the obvious places, you know, childhood experiences. But I’m not sure how it works in terms of causality. The good news is, if that’s the case, then anybody can get involved in service to other people at any step along the way. Of course, as a teacher of medical students, and of doctors, you want them to get involved in service to other people. That’s the whole point in medicine is to think about other people. And I’m convinced that people from all kinds of different backgrounds can do a good job at this.
Were you still at Duke the first time you traveled to Haiti?
Paul Farmer: No, I had just left. I graduated Duke, got some funding to go to Haiti at graduation, and I went afterwards. But I had written about Haiti and Haitians at Duke, but they were mostly migrant farm workers in the migrant farm workers stream that went from Florida all the way up to North Carolina and New York and beyond.
Was that seed planted back when you were picking oranges in Florida?
Paul Farmer: That’s speculation, ’cause I don’t know. I wasn’t the only person in my family who met Haitians back then, or got interested. I suppose the seed was planted. It would be easy to say that, but I’m not so sure. Is that fair enough?
It is tempting to say, “a” leads to “b” leads to “c,” but there’s a downside to doing that. I guess that’s what I’m saying here. If you believe that people are hard-wired to serve others, or that they have to have these experiences, then that excuses everybody else who hasn’t had any kind of experience like that from doing this, from engaging in public service. And I don’t want to do that ’cause I don’t believe in it. I’ve met kids from incredibly privileged backgrounds who have never known any personal hardship or material hardship, who nonetheless become splendid servants of other people, in medicine or nursing or any one of a series of — social work, et cetera — or development work. And they have nothing in common in terms of background. That’s the good news. Anybody can do this kind of work.
Who was Claude Lévi-Strauss, and what was his influence in your life?
Paul Farmer: He’s a famous anthropologist, cultural anthropologist. Actually the first time I left the country, except for Canada, was when I went to study abroad, in France in 1981, as a Duke student, and sat in on his classes. But again, it was more just the idea of, “Well, here’s a life of the mind, and someone who’s written lots of books, who’s a teacher, and maybe I could do that too.” It didn’t change the desire to be a physician, but it added sort of an academic discipline. I had professors at Duke who really set me on this path. Later, I would study with some anthropologists at Harvard, and do my Ph.D. under a medical anthropologist. So it was really not so much about the work itself, or his body of work, that ended up being of most interest to me in that field in anthropology. It was the idea of being a professor and writing books. That stuck with me.
What do you know now about achievement that you did not know when you were younger?
Paul Farmer: I think a lot of people, when they’re really young, and in their 20s, they are on their own quest for personal efficacy. And I understand that. It’s particularly true, I think, for young Americans. I mean, that’s the group I know best, obviously. But the sooner that people can discover that it’s really about building teams, and not about personal efficacy, I think the better — the more quickly — we can move forward. I believe that.
What do you see as the next challenge or the next great frontier in your field?
Paul Farmer: Well, I think that if I define my field as infectious disease, I’d say community-based care for chronic infectious disease, or new therapeutics are in the pipeline. If I define my field as public health, I would say strengthening health systems, right? But if I define my field more broadly, as development and social progress, I would say the biggest developments are going to be bringing together a growing movement around social justice, and linking that to the growing movement for environmental justice. I think once these things come together, that we’re going to see a lot of social progress in the planet. So yeah, any of those. That’s all optimism for you.
Do you think you were always destined to be an achiever? Do you feel you were any different than other kids?
Paul Farmer: No. I had a lot of opportunities, to go away to have a great education. But no. Working in the different countries over the last 25 years, I’m not so struck by difference. I’m more struck by similarity. This is a cliché, but people tend to be similar, in my experience. They have aspirations similar to our aspirations. So I’m more struck by similarity than by difference.
What advice or encouragement would you give to your grandchildren? What would you want to leave behind as your verbal footprint?
Paul Farmer: The most satisfying things that I’ve done — I’d like to use first person plural — that we’ve done, have been in service of other people. It shouldn’t be a secret. A lot of people say things like that. You can do all kinds of different things. Think of other people you’ve interviewed, or will be interviewing. Clearly, their areas of achievement are from all over the map. But whether you’re involved in basic science, or public health, or justice, it’s really, focusing on other people is a very satisfying thing to do. I mean that’s something that I would encourage anybody’s children or grandchildren is, get involved in work that is of utility to other people. And it doesn’t have to be your whole life, know what I mean? Say for example, you’re running a successful business somewhere. I’m not saying, give up your successful business and go be a social worker in — name the — you know, Los Angeles or Lisutu or whatever. What I’m saying is, some part of everybody’s life ought to be focused on this kind of work, ’cause it’s satisfying. That’s just, I think, good advice.
How do you define being an American?
Paul Farmer: I’m an American by birth, so I had all the birthrights of an American. Ability to speak my mind, ability to write and say what I wanted, the ability to go — I never worried about would I be able to go to high school. It never even occurred to me. That was just because I was born in the United States. It was only much later, when I went to other places and said, “Wow, they don’t even get to go to school.” Now that’s an embarrassing thing to confess. I should have been able to understand that, sitting right in my high school in Florida. But I didn’t. You just don’t know, and so the obvious definitions, those are definitions around the privilege of being born there. But you know, I would just say the ability to have those basic needs met, to be able to go to school all the way through — in my case, grad school and medical — but just to go through high school and know that you’re going to have something to eat at school. Or you’re going to be able to get your books.
Other people don’t really enjoy those freedoms. I would go ahead and call them “freedoms.” FDR called it “freedom from want,” as the fourth freedom, is freedom from want. I do believe, even someone of modest origins like me, still had freedom from want. I never experienced want. You asked me earlier about my childhood, living in a bus. But that’s not the same thing as living in a bus and having to run from violence, or not having enough to eat. It’s a very different kind of thing. So those are my sort of twin definitions of being an American, is a certain amount of protection from vulnerability around want. And then the civil and political liberties that we have. It’s terrific to be able to write what you want, and say you want and, and I’ve done that my whole life.
There’s a phrase you’ve used in the past, and we’d like to ask what it means to you. “If it’s in front of you, it has a reality.”
Paul Farmer: Did I say that? It’s true. I’m getting philosophical here. Humans, we have limitations, and we have limitations in terms of empathy and sympathy. And even the most gifted empaths in the world, it’s hard to imagine other people suffering. And so when it’s right there in front of you, it’s the most real thing in the world. I have a friend who says, “If you try to take a lollipop from a two-year-old, that lollipop’s the most important thing in the world to that two-year-old.” Well, I think you can be 50, and it’s still the same challenge. For example, isn’t it a failure of imagination that we can’t figure out what it’s like to be a woman who has no job, has a bunch of kids, doesn’t have safe housing? Shouldn’t we be able to figure that out? We should. But it’s not that easy to do.
The late Susan Sontag wrote a great essay about this. “Regarding the Pain of Others,” I think is the name of the essay. It’s a little book. She just lays it out there, very honestly. Some emotions she calls fragile and evanescent, like pity and compassion. Others less so, like solidarity.
We could take these failures of imagination, address them by trying to say, “Okay, this person isn’t in front of me, but that doesn’t make their suffering any less real. How can we try to attenuate suffering, regardless of where we are or how close we are to it?” I’ll give you an example that again is optimistic. I read somewhere that 45 percent of American households responded to the Asian tsunami. They have never been to Sri Lanka probably, right? That, to me, shows that if we cannot tap into that empathy and potential for solidarity, someone like me, then we’ve failed, because we have been right up against that suffering. We should be sharing that. We should find ways to make that real and vivid to everyone.
What is the effectiveness of having a government position versus working in the private sector?
Paul Farmer: I think what can be said about that is the same thing I’ve been talking about for years. Unless we can build public-private partnerships that support public health and public education, we’re going to get a lot of energy going into NGOs, but not really being able to be sustainable over time. And you know, again, back to growing up in the United States. It’s not like my parents built the school we went to as an NGO. We went to a public school. And there’s public water systems and public roads and public communications. Those are really important, and they’re no less important in Rwanda than they are in Florida. So finding a way to — regardless of whether you’re a university, whether the university’s an NGO, or Partners In Health is an NGO, and I can go down the long list of NGOs — we need to find a way to support public health and public education. And there are lots of other public goods that we could talk about. Those are the ones I know most about. And you know, I would put water in there. Do we really want to only be able to drink water out of a bottle, or do we want a public water system where you don’t get sick when you drink the water? And I would say, we need a public. We need public goods.
As a last question, what does the American Dream mean to you?
Paul Farmer: If you look back to the Depression of the 1930s… I would say that it’s hard to have an American Dream if you can’t get an education and you can’t feed your family. Again, I learned this as an adult, not as a child, because I was shielded from those problems as a child. I didn’t know that across the world, hundreds of millions of people would never enjoy education or basic health services. I didn’t know that. A big part of the American Dream for me is, again, yes, the ability to speak one’s mind, and the civil and political liberties that we enjoy there. But also, making sure that there’s some sort of safety net, so that people just don’t hit the ground and end up in the ground. That’s a big part of the American Dream in my view, is not having to worry if you’re going to not have another meal to eat, or not worrying that if you lose your job, then your whole family, you know, collapses into the poor house.
That’s something that’s worth fighting for. I think that’s what’s going on in the United States now, is people are saying, “Well, if unemployment hits ten percent, what do we do?” Well, in the Depression it was 25 percent, maybe more. And a lot of effort had to go into addressing the needs of the most vulnerable Americans then. That’s a big part of the American Dream. I think it’s worth restoring, and sort of rehabilitating, and talking more about that, about what was done after the Depression, during the Depression. What was done to say, “Hey people need not to be ill-clad, ill-housed and ill-fed.” The Second Bill of Rights, Roosevelt’s last inaugural — if I’m not mistaken, in 1944 — and he laid this all out very clearly. What did that mean, “freedom from want?” And he talked about, people ought to be able to get good jobs and good education and be safe, and I think that is a huge part of the American Dream. And people sometimes forget, we all forget. I get vivid reminders, because I go to places where there is danger and a great deal of want, and no sound safety net. So I get these reminders of what privilege we have. That’s really something that’s worth hanging onto.
Thank you, Dr. Farmer.
Paul Farmer: Thank you. Thank you very much.